Fighting on Two Fronts
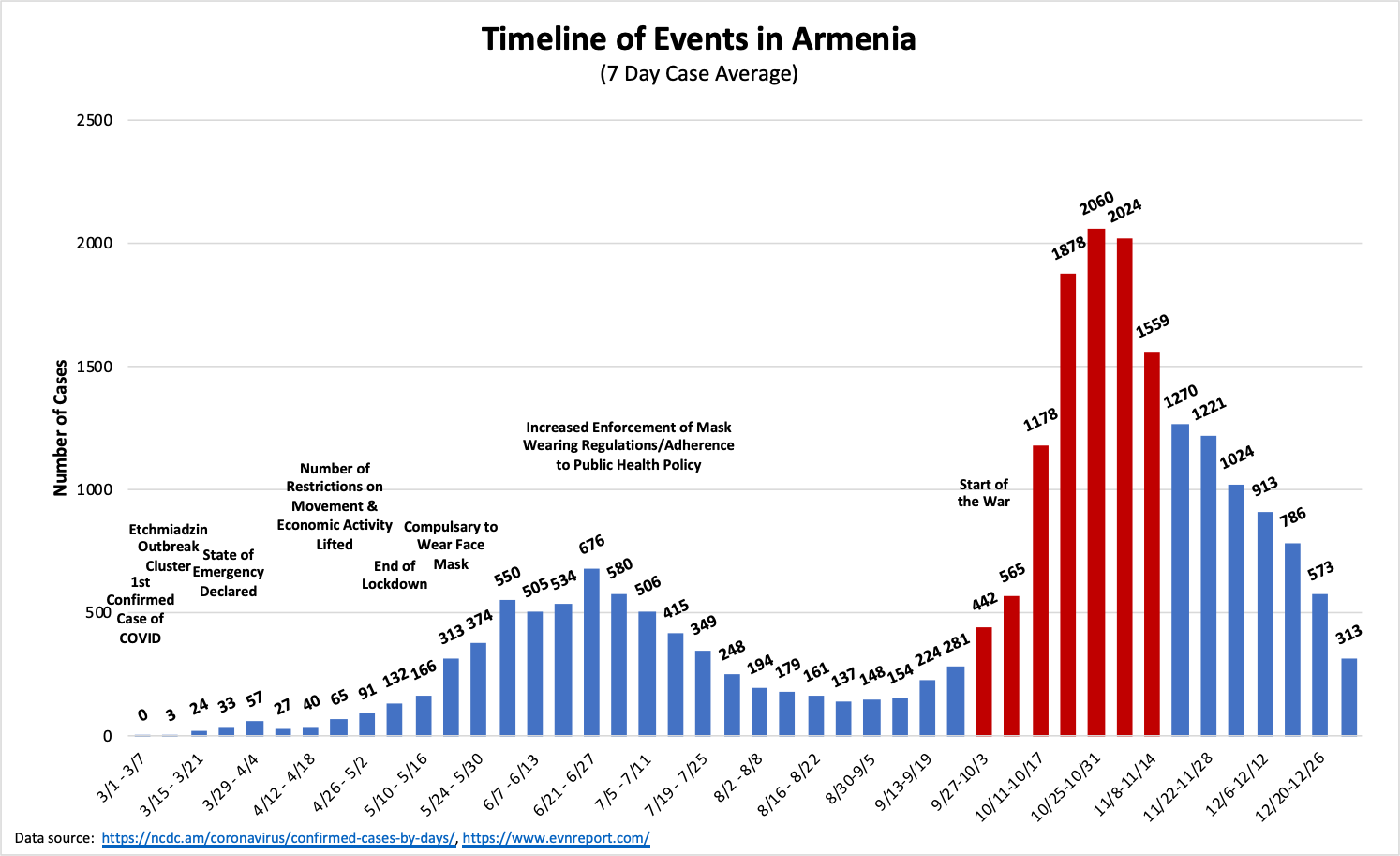
On September 27, 2020, Azerbaijan invaded Artsakh, launching a six-week nightmare in which every sector of Armenian society was mobilized for what was deemed an existential struggle for the survival of the nation. The war was fought not only along the line of contact, but also at hospitals against the backdrop of the deadly COVID-19 pandemic, bringing the healthcare system to the brink of collapse.
Armenia saw its first spike in COVID-19 cases during the summer. At the start of the pandemic, Armenia designated the Nork Infectious Diseases Hospital as the site for hospitalization of coronavirus patients. It implemented a government program of isolating and monitoring COVID-19 positive patients and their immediate contacts and instituted a national lockdown. Within two weeks of reopening the country in May, coronavirus cases began to rise rapidly. In response, the government expanded its capacity at the Nork Infectious Diseases Hospital, passed a mandatory mask mandate and created a strict enforcement arm to guarantee enforcement with preventative measures.
According to Dr. Kim Hekimian, the government of Armenia did a commendable job at managing the first surge of COVID-19 cases, efficiently expanding its hospital capacity and instituting preventative enforcement mechanisms to flatten the curve. Kim Hekimian, PhD is an Assistant Professor of Nutrition at Columbia University and co-organizer of the Armenian Public Health Working Group that coordinates global efforts to support the Armenian Ministry of Health in its COVID-19 response. In spite of the government’s efforts, the war precipitated an unprecedented spike in cases within the first two weeks after Azerbaijan’s invasion that dwarfed the initial surge and overwhelmed an unprepared health system. “Nobody could have foreseen either the war or the incredible increase in COVID cases as a result of the war,” she said.

The conditions of the war created new sources of spread of infection. For 44 days, the Azerbaijani military unremittingly shelled the towns and villages of Artsakh, destroying homes and businesses and killing and wounding civilians. The humanitarian crisis forced much of the population to flee, and those who stayed behind sought refuge in underground bunkers. These bunkers, with little air circulation and few opportunities for social distancing or habitual hand washing, were major sources of spread of COVID-19. Dr. George Melikian, an infectious diseases specialist from Los Angeles, California who volunteered at COVID-19 hospitals in Armenia during the war, shared that people who left Artsakh for Armenia partway through or at the end of the war often brought the coronavirus with them. “Most of the patients coming from Artsakh were COVID positive, the doctors and the patients, just because of all of the bunkering that was happening over there,” said Dr. Melikian.
Dr. Armen Hagopjanian attested to the impossibility of avoiding the spread of infection while bunkering down for survival. Dr. Hagopjanian put his life as a podiatric surgeon in Los Angeles on hold to travel to Stepanakert at the start of the war and perform surgeries on wounded soldiers and civilians. He tested positive for COVID-19 only after returning to Armenia, which he said was the case for most of his fellow doctors, surgeons and nurses at the Stepanakert hospital.
According to Dr. Hagopjanian, while doctors wore masks, they did not test incoming patients for COVID-19. “There are different priorities in a warzone,” he said. “A vast majority of patients brought to the hospital had either life or limb threatening injuries…Nobody cared about COVID while these patients were brought in. We were worried about saving their lives, saving their limbs, making sure they were stable, giving them enough blood, putting them on an ambulance and sending them back to Yerevan.”
Very little information is available regarding the incidence of COVID-19 within the Artsakh Defense Army. However, it is known that the coronavirus spread within the military and undermined its fighting capacity. Artsakh President Arayik Harutyunyan partly attributed the army’s weak fighting capabilities to the pandemic in a video broadcast the day after the signature of the ceasefire agreement codifying Armenia’s defeat. “The army was not in a good morale and psychological state,” he said. “The troops that were on the front line for 43 days were exhausted because of COVID-19, dysentery, etc. We did not have an opportunity to replace and to heal them.”
One source of the spread of infection was the movement of volunteer units of soldiers to Artsakh from Armenia, where the incidence of COVID-19 was much higher. Even if volunteers did not board buses headed for the frontline while exhibiting symptoms, a significant number of COVID-19 positive patients who are asymptomatic can still transmit the virus.
Community gatherings to bid farewell to soldiers departing for the frontline or grieve losses from the war rapidly transformed into superspreader events. Dr. Melikian affirmed that funerals were a major catalyst for the spread of the coronavirus among dozens of people at a time.
On December 28, 2020, 150 Armenian healthcare professionals from around the world published an open letter urging the Armenian church to implement mitigation measures, including the use of masks, social distancing and hand washing upon entry to prevent the transmission of the coronavirus during religious ceremonies and “help change the course of the pandemic in Armenia.” “The funerals that are meant for grieving and the meals that are meant to bring loved ones together, will allow COVID to spread, and turn into a death sentence for many,” the letter reads.
Enforcement of precautionary measures, which the government had deployed to successfully flatten the curve during the first surge of COVID-19 cases in the summer, also decreased in the fall. The daily tasks of enforcement units were quickly diverted to meet the needs of the war, Dr. Hekimian explained. The conditions of wartime not only increased exposure to the coronavirus, but also demolished the capacity to enforce measures to prevent transmission.
The particular consequences of the war for the spread of COVID-19 played out against the backdrop of longstanding issues of low health literacy and low levels of trust in official public health information. “There’s already a context of skepticism that has been a challenge for public health communication from Armenia from the beginning,” Dr. Hekimian noted.
Health literacy is the ability to obtain, understand and act on health information that is available to the public in order to make well-informed health-related choices. According to Dr. Hekimian, Armenia demonstrates low rates of health literacy. This problem is exacerbated by the dissemination of false information about COVID-19, a dangerous phenomenon the World Health Organization (WHO) has labelled the “infodemic.” Disinformation about COVID-19—including claims that the virus does not exist or that its vaccine is lethal—is broadcast in Armenia on television and radio stations as well as on social media, undermining the public health response and constituting a serious public health threat.
“Armenia needs to develop risk communication strategies and strategists,” Dr. Hekimian argued. “They need to build the skillset of people whose job it is to create messages with good formative research about what messages would be most resonant to pockets of people that are the most resistant to mask wearing.”
Even if the mechanisms to impose preventive measures like mask wearing and social distancing were preserved in wartime, the threat of the war overshadowed the threat of COVID-19. The first two weeks after Azerbaijan’s invasion were marked by an intensity of emotions that made it very difficult to think about protecting oneself from the coronavirus while mobilizing for the war effort. Even while Armenia battled on two fronts—the military front and the public health front—the clear and imminent existential danger posed by the former took precedence.

The massive spike in the number of COVID-19 patients requiring hospitalization already tested the capacity of the healthcare system. The combination of the spread of the coronavirus in wartime and the needs of wounded soldiers returning from the frontline placed an unprecedented stress on the health system, pushing it beyond its capacity.
While working at COVID-19 hospitals in Armenia, Dr. Melikian witnessed how facilities were running out of space while attempting to heal both infected patients and wounded soldiers. Waiting rooms were lined with mattresses where COVID-19 patients would rest until they could be admitted. “It’s this really grim situation where you’re waiting for somebody to pass away or get discharged, but more often to die so a bed would open up so somebody could get a bed,” he said.
One of the causes for the death of COVID-19 patients in Armenia is the strain on hospital capacity. The coronavirus moves through two phases of infection. During the first relatively benign week-long phase, the virus replicates in a person’s body. While most people recover during this phase, some enter a second dangerous period known as the cytokine storm, during which the body mounts an immune response by releasing inflammatory enzymes.
If a patient is admitted to the hospital early enough, doctors can give them oxygen and IV fluids in order to reduce the inflammation until they recover from the infection. However, in Armenia, a majority of people infected with the coronavirus were coming to the hospital late simply because there were no beds available for patients who were not extremely sick.
A second cause for the death of COVID-19 patients in Armenia is the inefficiency of the available oxygen modalities to treat patients with severe adverse outcomes. Patients in the cytokine storm phase require high flow oxygen at levels of 60 liters per minute. In Armenia the available technology delivers approximately 25 to 30 liters of oxygen per minute.
Dr. Melikian has been working with a team of doctors to improve how oxygen is generated and delivered. For example, he is involved with a project to provide hospitals with helmet vents that do not require high levels of oxygen flow in order to sufficiently oxygenate patients. These helmet vents cost about $200 each, an affordable option compared with other high flow machines that cost thousands of dollars.
Healthcare workers at COVID-19 hospitals in Armenia have been working nonstop through several coronavirus surges. The fatigue of working consecutive 24-hour shifts for a months-long period, combined with the pain of witnessing continuous deaths, has produced enormous psychological pressure.
Dr. Melikian attested to the adverse effects of the pandemic on the mental health of hospital workers in Armenia. “All the way up from the head of the hospital and the senior doctors all the way down to the nurses told me the same thing—they feel completely exhausted,” he admitted.
The compounded effects of the pandemic and war also have mental health implications for the population at large. Dr. Hekimian refers to national grief as a determinant of public health. Armenians are grieving the loss of family members and friends to the war and to coronavirus, the loss of homes and cultural heritage sites, the loss of land and the loss of public institutions.
“I believe very strongly that grief is associated with mental health and that mental health is associated with physical health,” she argued. “I believe that we will see consequences of health outcomes, COVID-related and non-COVID-related, to the national grief and mental health stress that everyone is experiencing in Armenia at this time.”

On March 23, 2020, in the early weeks of the pandemic, the United Nations Secretary General António Guterres issued a call for a “global ceasefire.” In June, 170 countries endorsed his appeal, and in July, the UN Security Council unanimously adopted Resolution 2532 expressing its support for a global ceasefire for the duration of the pandemic.
On October 22, nearly a month into the war in Artsakh, the WHO published a statement warning that the violence had severely accelerated the transmission of COVID-19. “The conflict is causing a direct disruption to health care, further burdening health systems that are already stretched by the pandemic,” the statement read. “An immediate cessation of hostilities is vital to preserve access to health services—a fundamental human right.”
Azerbaijan was conspicuously absent from the list of signatories to the March 23 ceasefire appeal (which Armenia did sign). Health professionals and political leaders have noted the opportunistic timing of the invasion, as the attention of the world was consumed and Armenia’s resources were diverted by the pandemic. Azerbaijan’s well-timed attack on Artsakh succeeded in spreading the virus amongst soldiers and civilians, overwhelming the health system and increasing the suffering of a population already fatigued by a months-long pandemic.
Considering the present statistics, prevention is the only thing that will flatten the curve until a vaccine is widely available. “It’s really incumbent upon every donor humanitarian assistance group…to make sure that they are also distributing, in addition to food, that they are distributing masks and hand sanitizer and giving people the agency and autonomy to be able to adhere and prevent themselves from getting sick,” Dr. Hekimian asserted. “There has to be a collective unity of messaging and collective unity of understanding that these measures, though very difficult to do and adhere to vigilantly, they are needed in order to build Artsakh stronger.”
In the meantime, Diasporans can support the healthcare workers toiling to heal infected patients and wounded soldiers and civilians. This fundraiser, organized by Mary Minassians, is raising money to donate high flow machines to hospitals in Armenia in order to deliver oxygen to COVID-19 patients. People can also donate to Eternal Nation, a foundation created by Dr. Hagopjanian, which aims to provide comprehensive rehabilitative healthcare to injured Armenians.










Lillian ~ Your bravery and commitment to revealing the truth-of-the-moment suggests to me that you are the real-life embodiment of the young women portrayed in the new novel “Armenia’s Fingerprint”. Please go to Amazonbooks.com and look it up. If you wish, send me your address and I will send you a signed copy immediately. I thank you heartily for your journalistic expertise and courage. May I share your article on my website? It moved me greatly.
Bruce David Badrigian